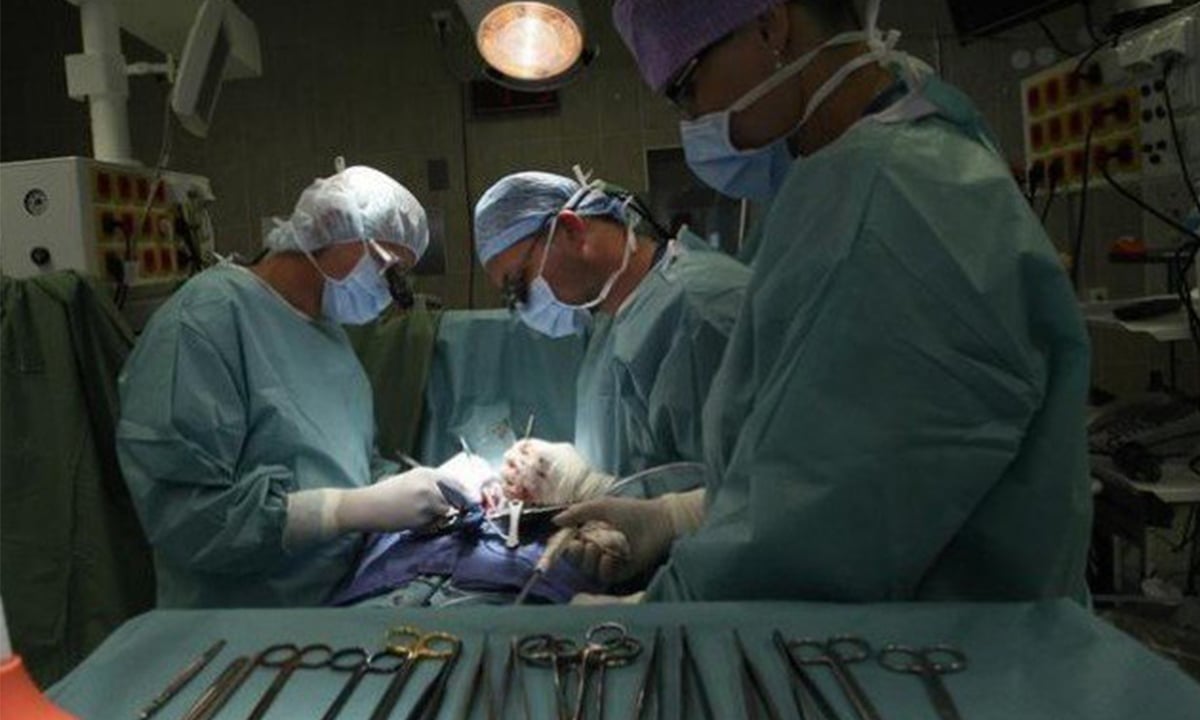
Newspapers and television channels have reported several cases of medical negligence last month. In perhaps the most widely reported among them, a nine-month-old girl died at a private hospital in Karachi’s Gulistan-e-Jauhar area on April 15 after she was given a wrong injection. A week or so later, a quack reportedly administered a wrong injection to another child in the same city, leading to the child’s death.
Towards the end of the month, news media was flooded with reports that a large number of children have been found to be HIV positive in Sindh’s Larkana district, allegedly due to illegal and hazardous medical practices prevalent there.
These incidents can be attributed to two broad causes: medical malpractices and professional negligence. The distinction between the two is important. The latter is an act by a qualified and trained healthcare provider who deviates from scientific practices and standard operating procedures, resulting in injury or permanent damage to his or her patients. The former is an act of illegal use of medicine, skills or equipment by an unqualified person impersonating as a healthcare provider — a criminal act that endangers lives.
Before we proceed to discuss how to tackle these two problems, we need to be clear that medical or surgical negligence by qualified and trained professionals is not uncommon. Cases involving this kind of negligence have been reported not just from developing countries like Pakistan but also from the developed ones. For instance, between 44,000 and 98,000 fatalities reportedly occur in the United States every year due to mistakes by medical workers. The United Kingdom’s National Health Service was, similarly, reported to have dealt with 5,609 claims of clinical negligence and 3,766 claims of non-clinical negligence in 2004-05.
The findings of a 1984 study that reviewed 30,121 randomly selected patient records from 51 randomly selected acute care hospitals in New York state suggest something similar. The review showed adverse impacts of hospitalisation in 3.7 per cent of all the records examined. Out of these, 27.6 per cent adverse impacts were caused by some kind of negligence.
There is no way to develop a healthcare system where there are no errors, no negligence. Human beings are not perfect so some errors are bound to happen even in the most efficient of the human-devised systems.
The menace of quackery, on the other hand, is mostly a developing world phenomenon. Illegal medical practices are quite common not just in Pakistan but also in the rest of South Asia, and as well as other parts of the globe. These can certainly be eradicated through effective administrative mechanisms.
Pakistan’s healthcare system, however, is neither equipped to deal with medical negligence nor does it have efficient institutional arrangements in place to get rid of quacks. While it does not ensure that legitimate healthcare providers always follow scientific practices and protocols, it also has no effective way to stop unqualified people from impersonating doctors.
Admittedly, there is a dire need to reorganise Pakistan’s entire healthcare system. We not just need to control and minimise the incidents of medical negligence, we also need to remove the loopholes that healthcare regulation and administration suffer at the grass roots level.
To achieve these twin objectives, Pakistan must look into its medical training and healthcare delivery system. It must also make strong institutional arrangements for monitoring and quality control of medical and paramedical training. Similarly, healthcare administrators should look into duty hours, work ethics and work commitments of medical professionals as possible reasons for negligence and malpractices and address these problems as effectively as possible.
Some other much-needed steps include the protection of legal rights of both doctors and patients and the provision of financial and administrative autonomy to the Pakistan Medical and Dental Council (that oversees doctors and dentists in the country) and healthcare commissions (mandated to regulate clinics and hospitals).
It is equally important to ensure that doctors and other medical practitioners working in the government sector are paid well and their service structure is devised in such a way that it rewards hard work, merit and seniority in equal measure. At the same time, there should be mandatory assessments of their professional competence at regular intervals.
Most crucially, Pakistan must increase its current level of spending on healthcare – which stands at less than one per cent of the Gross Domestic Product (GDP) – to four to six per cent of its GDP. Most of this money should be spent on putting in place a corruption-free healthcare delivery system in the public sector in order to benefit the people of the country — and not just a rich and privileged elite.
The writer is the chairman of Sindh Health Care Commission.
This article was published in the Herald's May 2019 issue. To read more subscribe to the Herald in print.